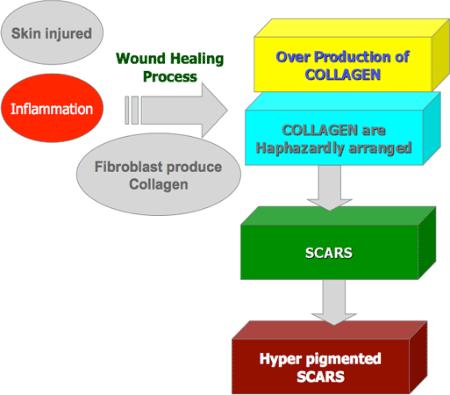
UNDERSTANDING WOUND HEALING
The following happens in the wound healing process before you start to see scars.
|
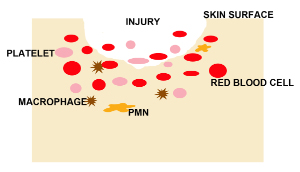
Hemostasis
– Immediately after injury |
Vascular and cellular responses
Release of cytokines – pDGF, TDGF-β, eGF
Vascular constriction – lasts for 5 – 10 minutes
Fibrinoplatelets deposited to stop bleeding
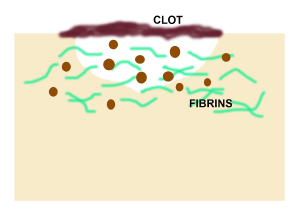
Clot formation
Wound edges are still not united – wound still open
|
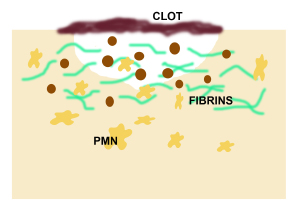
Inflammation
– happens after injury |
Can last from 1 – 5 days
Experience of swelling, pain and redness
Early inflammation– feeling of pain, warmth and edema
Plasma fluid & protein, antibodies, leukocytes and red blood cells enters the injured area.
Late inflammation– micro circulation slows down
Histamine, serotine, protoglandins appear
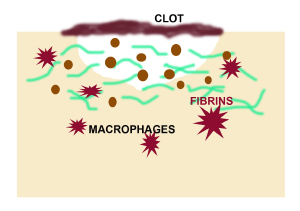
Neutrophils & monocytes move towards wound area to ingest wound debris
The repair process starts
|
Proliferation
– starts at about 72 hours after injury |
Reconstruction of injured tissue
Lasts from 2nd to 20th day approximately
Growth factors are released
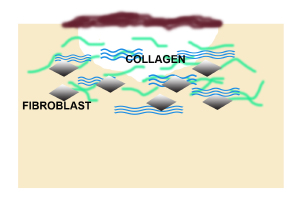
Fibroblasts begin to produce collagen at the wound area
Main types of collagen produced are types I & III (80% type I)
Formation of the extracellular Matrix (ECM) and granulation tissues
Angiogenesis occurs – capillary growth into the ECM
Cellular structure is regenerated
Collagen forms to give wound tensile strength
Re-epithilization starts by the 3rd week
Process of contraction is almost complete
Rate of collagen deposits slows down after about 3 weeks from injury
Remodelling of collagen deposited occur for months after injury
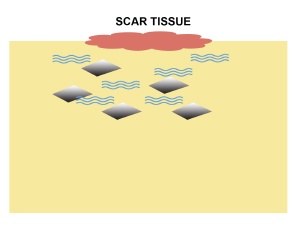
Excessive mass of collagen and ground tissue cause formation of scar
SCAR TYPES
There are basically 4 types of awful scars
| Keloids |
Hypertrophic scars |
| Hypotrophic scars |
Post Inflammatory Hyperpigmented scars |
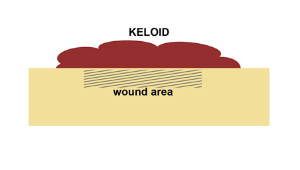
Keloids
Very thick clusters of scars formed from excessive tissue
The appearance of the scars is often red or purplish in color
Keloids often grow and extend outside of the wound area
Keloids are very difficult to treat and have a tendency to reappear after treatment
Various treatment methods include corrective surgery and steroid injections
Hypertrophic Scars
|
Thick, red and raised scars
Hypertrophic scar tissues remains within the boundaries of the wound area
They can be improved with scar removal methods
|
Hypotrophic Scars (or Atrophic Scars)
|
Hypotrophic scars appear sunken, formed a depression below the skin level
These scars form from deficiency in tissue formation
Example: Acne scars; Chicken pox scars
Hypotrophic scars can be improved with dermabrasion or laser therapies |
Post Inflammatory Hyperpigmented Scars |
These scars are pigmented but not raised ore sunken
Can be avoided with early prevention
Existing pigmentation can also be improved |
SCAR THERAPIES
There are many modalities of scar treatment & management
The following are examples:
| WOUND HEALING PROCESS AND CONVENTIONAL SCAR THERAPIES |
Reducing the risks of bad scar formation
|
It is better to avoid bad scarring before the scars appear.
Risks of bad scar formation can be reduced with early care and attention to the wound area.
Apply Cybele Scagel as soon as the wound closes (upon complete epithelization)
Should bad scars start to appear, doctors may advise additional methods of scar management
In some cases, corrective surgery or other invasive methods may be required to improve the scars.
|
| SCAR CARE WITH CYBELE SCAGEL IN SCAR MANAGEMENT |
EXAMPLE OF CYBELE SCAGEL USED IN COMBINATION THERAPY
|
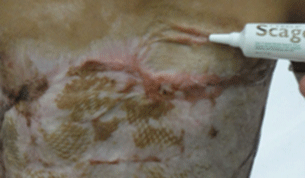
Closed wound and scarring from burn incident
|
Care for the skin by applying Cybele Scagel
|
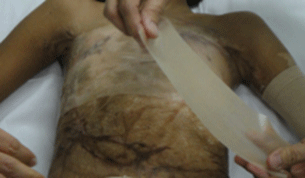
Combining use of silicone gel sheet after Cybele Scagel
|
Ensuring the silicone gel sheet is applied properly
|
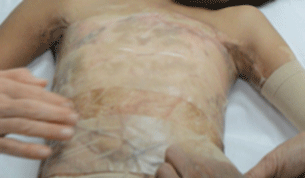
Using elastic bandage to hold the silicone gel sheet in place
|
Additional combination with presure therapy by using pressure garment
|